INTRODUCTION
Close to 30% of all cancer deaths are due to lung cancer1. Lung cancer screening (LCS) with low-dose computed tomography (LDCT) reduces lung cancer mortality2,3. The National Comprehensive Cancer Network (NCCN) and US Preventive Services Task Force (USPSTF) guidelines recommend LCS in high-risk patients, as do a number of other professional organizations4,5. The USPSTF recommends screening current and former smokers aged 55–80 years who have smoked ≥30 pack-years, and who quit within 15 years if a former smoker. Although there is limited information on the proportion of high-risk people who undergo LCS, Pinsky and Berg6 estimated, using National Lung Screening Trial (NLST) criteria, that 6.2% of adults over the age of 40 years would be eligible for screening6. Yet, the number of patients screened at most LCS centers is anecdotally very low. We recently reported that only 8% of primary care physicians reported referring most or all high-risk patients to an LCS center during the prior 12 months7. A number of barriers to utilization of LCS in high-risk patients exist.
We recently conducted a survey of primary care physicians (PCPs) and identified that concerns regarding the effectiveness of LDCT to prevent death from lung cancer, potential risks of LDCT, and costs of LDCT were of greatest concern to PCPs7. We also identified that few PCPs have a mechanism to identify patients eligible for screening in an automated fashion because of the way that tobacco exposure is documented in the electronic medical record (EMR). We reported that capturing a detailed tobacco exposure history in the EMR improved utilization of LCS and tobacco cessation services8. Novel systems approaches are needed to overcome barriers and improve utilization of LCS.
In addition to the life-saving potential of early detection of lung cancer, LCS offers additional value by serving as a point-of-entry into tobacco cessation counseling for current smokers. Integration of tobacco cessation into LCS programs is mandated by the Centers for Medicare Services (CMS). Although a recent small interview study reported that a large proportion of current smokers expressed that LCS might lower their motivation for tobacco cessation9, data from the National Lung Screening Trial and from the International Early Lung Action Program have shown that LCS stimulates tobacco cessation and that cessation rates are highest among patients with abnormal screening test results10-12.
A far larger number of current smokers seek out tobacco cessation services, such as telephone quitlines, tobacco cessation groups, or individual counseling, compared with the number of smokers screened with LDCT. For example, Davis et al.13 reported that 363656 calls were made to state quitlines over a 12-week period in 2012. Yet, most tobacco cessation services offer no education on LDCT. Moreover, the vast majority of smokers who are eligible for LCS and seek out tobacco cessation services do not know about the potential benefits of LDCT14. Education by tobacco cessation counselors on the benefits of LDCT and where to be screened, may be an important way to improve adherence to LCS guidelines. Questions regarding the effectiveness of this approach warrant investigation. These include the feasibility of LCS education in a variety of tobacco cessation counseling settings (one-on-one counseling, group counseling, telephone quitlines, and online courses) and the type of education that is most effective, but still within the scope of practice of the counselor.
In this study, we explored the feasibility of training tobacco cessation counselors in a large health system to educate smokers, attending group tobacco cessation classes, on lung cancer screening within a large health system.
METHODS
Current smokers who attended at least one tobacco cessation group session, part of a four-session course entitled ‘Freedom from Tobacco,’ at one of two participating Kaiser Permanente medical centers in Southern California, were eligible to participate during May 2019. A total of 25 volunteer participants completed surveys at the end of the class after distribution of the survey by tobacco cessation counselors. No class participant declined to complete a survey. Anonymous surveys were completed on paper forms and completed surveys were collected and mailed to City of Hope for analysis by study staff. Participants were not compensated for survey completion. This study was reviewed and approved by the Kaiser Permanente Institutional Review Board. A waiver of informed consent was obtained as protected health information was not collected as part of the survey.
Training of tobacco cessation counselors
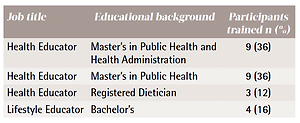
Four tobacco cessation counselors at two sites, where group tobacco cessation counseling was offered, administered the study educational intervention. The training backgrounds of the counselors are summarized in Table 1. The counselors were trained on lung cancer screening by the principal investigator by reviewing detailed information about the data supporting lung cancer screening, and details about eligibility requirements, risks, harms, and logistics including how patients can get screened and insurance coverage. The counselors were then provided with a script in outline form on the content to deliver during tobacco cessation classes. In addition, printed patient education material was reviewed with cessation counselors and they were instructed to distribute this material to participants receiving the educational intervention for reinforcement. Upon completion of the pilot program, the cessation counselors were contacted regarding their experience and to provide feedback to the study team.
Survey items and measures
The survey was structured into five parts, and took approximately 5 minutes to complete. First, participants were asked how much the information provided helped with understanding various aspects of lung cancer screening including benefits, risks from how screening is done, eligibility criteria, insurance coverage, and who to contact for more information about LCS using a Lickert scale of 1–5. Participants were then asked about whether the amount of information provided was the right amount and how satisfied they were with answers provided by cessation counselors to any questions asked. An open-ended question soliciting comments about the intervention was also included. Finally, sociodemographic characteristics including age, race, income, education, and smoking history were collected.
Data analysis and statistics
Descriptive statistics including counts and percentages were used to summarize participants’ sociodemographic information, current smoking status, and opinions about the amount of information provided about lung cancer screening. Responses regarding understanding of the components of LCS education were summarized as median of the Lickert scale response. For questions pertaining to satisfaction with answers to questions asked, results were summarized after being grouped into agree/strongly agree and disagree/strongly disagree categories. Any differences between the study sample and the combined totals in Tables 2 and 3 are due to missing data.
Table 2
Sociodemographic characteristics and smoking history of study participants
Table 3
Response to survey questions
RESULTS
We included 25 smokers in the analysis. Their sociodemographics are summarized in Table 2. Most participants (72%) were aged 55–80 years, the age range for LCS eligibility. The median pack-year history of smoking was 40, and 64% of participants had a smoking history of 30 pack-years or greater. The population was racially/ethnically diverse. Participants had varied educational backgrounds, with 32% of participants completing some or all of high school as their highest level of education. Four participants (16%) reported that they had previously undergone lung cancer screening.
Overall, the intervention was well received. The median score for the understanding of all components of the intervention was 5 (‘completely understand’). Most participants (92%) felt that the information provided about LCS was the right amount, while the remaining few participants felt that there was too little information. In addition, most participants (88%) were satisfied with the answers that the cessation counselors provided to questions asked during the session. No survey responder provided any specific comments about their experience or suggestions for improvement on the survey in response to the open-ended questions asked about the educational intervention.
We re-analyzed the study data after restricting our analysis to 21 participants who responded that they had never undergone lung cancer screening. Results were similar to the over group with regards to median score for understanding of the components of the intervention (5), the amount of information provided during the intervention (90% reported the right amount of information provided), and satisfaction with answers to questions asked (86% very or somewhat satisfied).
DISCUSSION
The study suggests that it is feasible to train tobacco cessation counselors to educate smokers, attending group tobacco cessation counseling classes, about LCS. Education provided in this study was both understood and well received by the large majority of smokers surveyed. This is the first study to our knowledge investigating the feasibility of training tobacco cessation counselors to educate smokers about LCS. There is considerable effort to incorporate tobacco cessation into lung cancer screening programs12,15. In the United States, tobacco cessation services are required for sites in order for reimbursement to be given by the Center for Medicare and Medicaid Services (CMS). A number of studies have been published evaluating different modalities of tobacco cessation counseling for patients undergoing LCS16-20.
While use of LCS as a teachable moment for tobacco cessation is important, far less has been known about use of tobacco cessation as a teachable moment for LCS. A far larger number of smokers seek out tobacco cessation services than LCS7,13. While educating smokers on LCS, which is recommended by the U.S. Preventive Services Task Force and the American Cancer Society, may be well-intentioned, there are several issues that should be clarified. Again, our study shows that it is feasible for tobacco cessation counselors to administer education regarding lung cancer screening. While the U.S. Public Health Service recommends tobacco cessation counseling training for all healthcare professionals, the educational and training background of cessation counselors providing most cessation services can vary21. There are other important issues that need additional investigation, including what kind of LCS education and how much information should be administered. LCS education can be given in person, by telephone, or through video or online content. The format of education and length of the educational intervention may also depend on the type of cessation counseling that is administered, i.e. one-on-one, group counseling, phone counseling, or online counseling. Most importantly, the effect of the educational intervention on utilization of LCS has not been determined. It is also unclear whether such educational intervention has an effect on abstinence from tobacco. Several studies have shown that participating in LCS does not lead to increased smoking rates, and may lead to increased smoking cessation rates11,22, but it is not known whether LCS education affects tobacco cessation rates in those seeking tobacco cessation services.
Limitations
Our study has several limitations. First, it is a relatively small study at two sites administering group tobacco cessation classes within a single healthcare system. These results may differ in other tobacco cessation settings, such as phone counseling. Although the number of participants was small, it was fairly diverse with respect to race/ethnicity and educational background, which should make this generalizable to most US populations. In this study, we explored the feasibility of a brief LCS educational intervention that included printed literature for the participant to take home. More extensive educational interventions may result in different acceptance than what we found. Finally, this study was designed only to test feasibility of the intervention in this patient population. Additional studies are needed on the effect of an LCS educational intervention that is delivered by tobacco cessation counselors, at the time of tobacco cessation counseling, on LCS utilization and tobacco cessation rates.